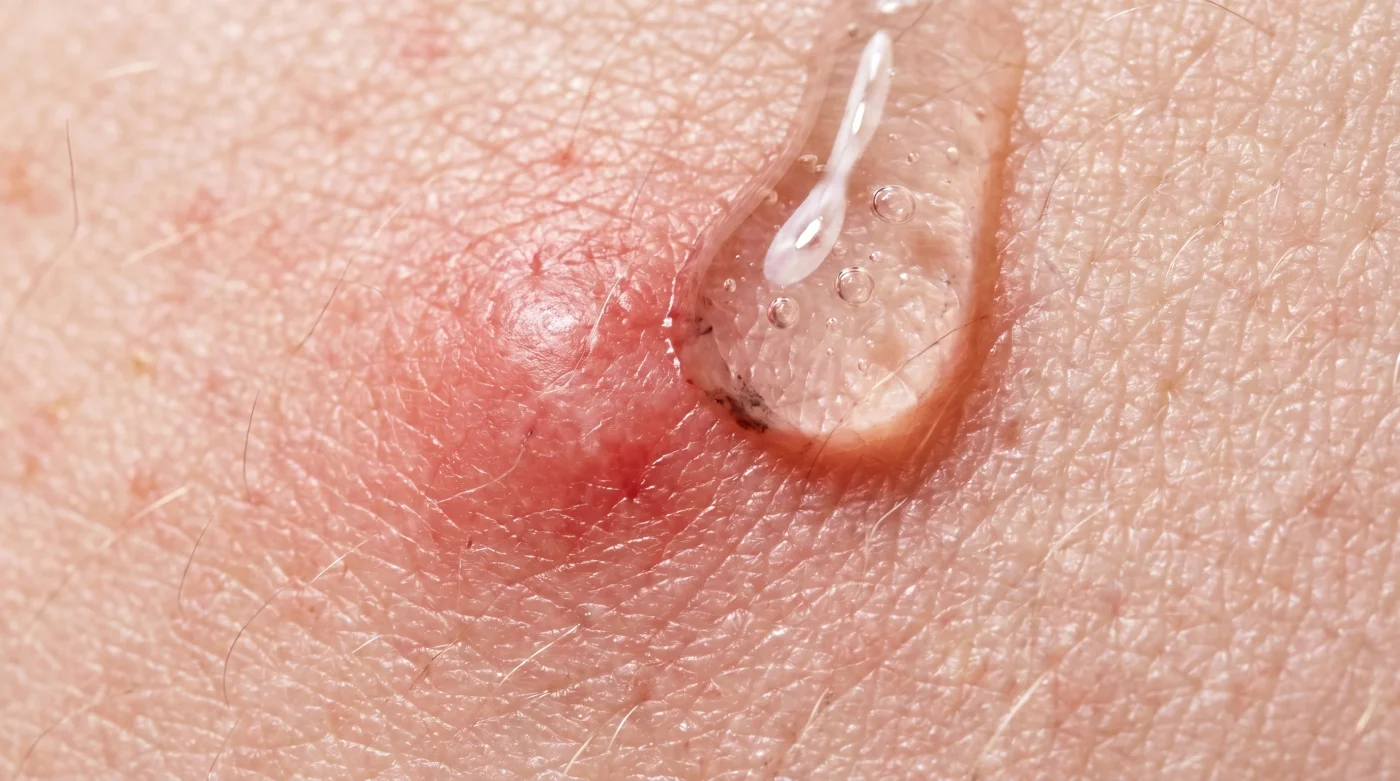
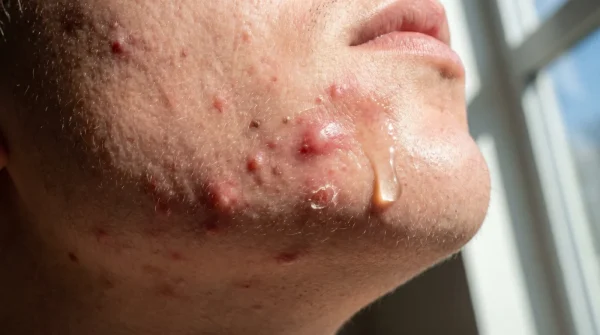
The bathroom is quiet, save for the dull hum of the exhaust fan. The harsh overhead light casts long shadows across your face as you lean toward the mirror. A new, painful blemish has surfaced along your jawline, throbbing slightly in time with your pulse. You know this routine by heart.
You reach for the tiny, potent tube sitting on the shelf. The clear gel feels cold on your finger. You dab it directly onto the swelling, pressing it in, waiting for the familiar stinging sensation to arrive. We equate pain with progress, trusting the sharp bite of a spot treatment as proof that the formula is working.
You wake up the next morning. The bump might be slightly flatter, but the skin surrounding it is angry, tight, and already settling into a stubborn purple-brown hue. For years, the beauty industry has convinced you that aggressively drying out a blemish is the fastest route to clear skin. But what if the very remedy you apply is permanently stamping the ghost of that breakout into your complexion?
The Burn Paradox
Think of a fresh breakout not as a pest to be eradicated, but as a tiny, isolated fever on your face. When skin is inflamed, its natural defenses are already operating in a state of high alert. Blood rushes to the area, and the delicate moisture barrier is temporarily compromised as the pore swells.
Introducing a concentrated beta hydroxy acid directly onto this vulnerable tissue is like pouring salt on an open wound. You are not gently exfoliating the pore; you are triggering an acute trauma response. The acid strips away whatever fragile protection the skin had left, creating a microscopic chemical burn.
The perspective shift happens when you realize the dark spot left behind is not a scar from the pimple itself. It is post-inflammatory hyperpigmentation caused entirely by the intense, localized distress of the spot treatment. Melanocytes—the cells responsible for skin pigment—panic under the acute stress of concentrated acids on broken skin. The blemish would have faded in a week, but the dark mark you created by burning it will take months to clear. We need to stop attacking the skin and start coaxing it back to baseline.
The Dermal Researcher’s Secret
Dr. Aris Thorne, a dermal researcher based out of a quiet Vancouver lab, spent her early thirties battling what she assumed were terribly stubborn acne scars. “I was spot-treating every minor bump with a 2 percent salicylic acid gel,” she noted during a crisp October morning over coffee. She discovered through her clinical trials that melanocytes act like nervous sentinels. By aggressively drying the surface of an active breakout, she was literally baking the pigment into her dermal layers as a defense mechanism against the acid. When she swapped her harsh spot treatments for gentle, full-face barrier support, her permanent marks faded within a single season.
Rethinking the Acid Approach
We all have different thresholds for skin trauma, and how you adapt this new understanding depends entirely on how your skin responds to stress. Here is how you pivot based on your specific complexion profile.
For the Chronic Picker
If you cannot keep your hands off a breakout, a spot treatment is the worst thing you can apply to an open, weeping pore. Instead of acid, your skin requires an artificial scab. Hydrocolloid patches absorb the fluid while protecting the raw tissue from oxygen and bacteria, preventing the dark crust that leads to hyperpigmentation.
For the Red and Reactive
When your breakouts arrive with intense, throbbing redness, heat is your primary enemy. Applying acid here will immediately trigger pigment production. Focus on drawing heat out. Cool compresses and centella asiatica offer a better, calmer route to reducing the swelling without waking up the melanocytes.
- Makeup sponges actually remove coverage when used completely soaking wet
- Magnesium supplements clear hormonal acne faster than topical spot treatments
- Liquid foundation accelerates visible aging for women over forty years
- Rice water scalp treatments are destroying your natural hair elasticity
- Vitamin C serum works backward if applied after this product
- Oliver Bonk hockey hair revival sparks a massive salon styling trend.
- Snail mucin allergies are silently causing your sudden adult cystic breakout.
- Dianna Russini camera makeup routine uses a drugstore primer for sweatproof foundation.
- Peptide lip treatments cause permanent volume loss when used daily.
- Health Canada Sephora investigation forces immediate removal of viral acne patches.
For the Congested but Calm
If your skin suffers from closed comedones—those stubborn, flesh-coloured bumps that never come to a head—salicylic acid remains incredibly useful. The trick is to use it as a widespread, low-percentage preventative wash or toner, rather than a concentrated dab on a single spot.
The Mindful Application
Managing a sudden blemish requires a quiet, methodical touch rather than a panicked attack. You want to support the healing cycle, not interrupt it with chemical warfare.
Start by abandoning the magnifying mirror. Back away from the glass. If you cannot see the spot from three feet away under normal room lighting, nobody else can either. Here is how you handle the arrival of a new blemish.
- Cleanse the area with a gentle, non-foaming wash using only tepid water hovering around 30 Celsius.
- Apply your standard, barrier-supporting moisturizer over the entire face, including the blemish, letting it act as a buffer.
- If the spot is a whitehead, apply a simple hydrocolloid patch to drain it safely overnight.
- If it is a deep, blind pimple, dab a tiny amount of a sulfur-based paste to calmly reduce swelling without burning the tissue.
The Tactical Toolkit:
- Temperature: Keep water lukewarm; hot water exacerbates inflammation and signals melanocytes to wake up.
- Wait Time: Let your moisturizer sink in for five full minutes before applying any targeted patch or paste.
- Ingredients to shelf: High-concentration BHA spot gels and drying lotions loaded with isopropyl alcohol.
A Truce with Your Complexion
Letting go of the aggressive spot-treatment routine feels deeply unnatural at first. We are conditioned to desire the immediate, visible destruction of our perceived flaws, measuring success by how dry and flaky the blemish becomes.
Yet, there is profound peace in stopping the daily chemical warfare against your own face. When you stop burning away your blemishes, you stop creating the dark marks that haunt your reflection long after the breakout has passed.
You move from a cycle of punishment and concealment to one of patience and support. It turns out that the secret to a clear, even complexion is not finding a stronger acid. It is having the grace to let your skin heal on its own terms.
“Your skin is an organ, not an opponent; treat a breakout as a plea for support, not a target for eradication.”
| Key Point | Detail | Added Value for the Reader |
|---|---|---|
| The Burn Response | High-concentration BHAs damage inflamed tissue. | Prevents you from creating dark marks out of temporary blemishes. |
| Melanocyte Panic | Pigment cells overreact to acidic trauma on broken skin. | Helps you understand why scars seem to last for months. |
| Barrier Support | Using hydration instead of acid to heal spots. | Speeds up actual recovery time while maintaining skin health. |
Frequently Asked Questions
Does this mean I should throw away all my salicylic acid?
Not at all. Salicylic acid is brilliant at keeping pores clear when used as a gentle, low-percentage wash or liquid exfoliant across the whole face. It only becomes problematic when concentrated directly onto an already inflamed, broken blemish.
How long do post-inflammatory hyperpigmentation marks last?
Depending on your skin tone and cell turnover rate, these dark marks can linger anywhere from three months to over a year. Preventing them by avoiding chemical burns is far easier than trying to fade them later.
What is the best alternative to a spot treatment for a painful pimple?
A dab of a gentle zinc oxide cream or a sulfur paste can reduce inflammation without triggering a burn response. Hydrocolloid patches are excellent for whiteheads.
Why do companies sell spot treatments if they cause dark marks?
They deliver immediate gratification. Spot treatments dry out the top layer of the blemish quickly, making it look temporarily flatter, which satisfies the consumer’s desire for fast action, even if it causes long-term pigmentation issues.
Can I use a spot treatment if my skin is very resilient?
Even resilient skin has a breaking point. While you might not scar as darkly as someone with reactive skin, you are still prolonging the healing process by damaging the localized moisture barrier.